I’ve had some really great questions come my way since starting this blog series. I was not able to address all the questions within my past two entries, so I decided to dedicate one post to responding to questions and concerns of our readers. I hope this addition is helpful and informative. If you continue to have any questions or concerns, please email me at [email protected] or visit our clinic website to schedule an appointment: https://beyondbasicsphysicaltherapy.com/
Question:
I just had my first baby 9 weeks ago and think I may have a Diastasis Recti. How can I check if I have one?
– D.M., FL
Answer:
A small separation is normal for everyone. Although standardized norms are still yet to be determined, generally a 2 cm separation at and above the belly button and a 1 cm separation below the belly button is considered typical. Most people don’t have a caliper for an accurate measurement and using a ruler to measure on yourself can be tricky. An easy cheat is to use your fingers. Two finger widths above and at the belly button is average and 1 finger width below is average. It can be hard to feel the edges of the muscles when relaxed, so measuring first while lifting your head and bringing your ribcage towards the pelvis is often easier. You want to measure at three different locations along the linea alba: At the belly button, 3-4 inches above the belly button and 3-4 inches below the belly button. The separation is often different at each location and knowing where your separation is can help direct where you should be splinting your abdominals during the exercises.
Start by lying onto your back with both knees bent. Take one hand and place your fingers at your belly button aligned horizontally (see picture below). Press into the tissue with moderate pressure so that your fingertips are past the depth of the skin. Lift your head off the floor and slowly bring your ribcage towards your pelvis. When you feel your muscles start to pop into your fingers, stay in that position and take note of how many fingers fit within the gap. If you do not feel the muscles either move more into the crunch, press until the tissue with more pressure or increase the number of fingers (The separation may be wider). Lay your head back down and repeat at 3-4 inches above and below the belly button.
Question :
Is a diastasis recti the same thing as a hernia?
– J.R., NY
Answer:
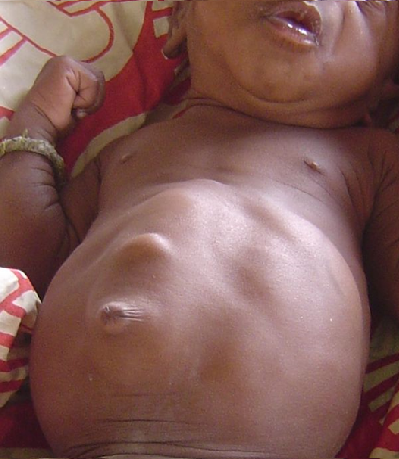
Great question. A hernia and a diastasis recti are not the same thing. The lina alba consists of multiple fascial layers and while one layer may be overly stretch, the others may still be intact. With a diastasis recti, the rectus abdominis muscle separates from a widening of the linea alba, but the stretched and thinned linea alba still holds in all the abdominal contents. A hernia is when there is a hole in the abdominal wall and the abdominal contents are pressed outwards through the hole. The below picture is a great example of an infant with both a diastasis recti AND a hernia. You can see the separation of the muscle in the front (football shaped bulge) as well as a hernia (circular bulge above belly button) coming through the diastasis.
Question:
I had surgery a while ago for ulcerative colitis. I had an incision from just above the belly button to about 3 inches below. I used to have good abs but I’m struggling to get them back especially towards to lower abs. I can feel some separation in the middle of the muscles of my core and am wondering if that’s part of the problem. I was hoping you might have some advice. I’m desperate to get my flat tummy back. I don’t need a 6 pack but I do miss having a flat tum. Would really appreciate your thoughts.
– A.H., UK
Answer :
Having any surgical incision along the linea alba definitely compromises the integrity of the closed canister and often leads to a diastasis recti. Studies have shown that almost 100% of women with laparoscopies (just a small hole) through the belly button or along the linea alba are left with a separation, so a longer incision line would almost definitely leave you with one. The separation could definitely be contributing to your difficulty with getting your flat tummy back. I would stay away from crunches right now, but start introducing some TA (Transversus Abdominis) exercises with abdominal splinting that I discussed in part 2 of this blog. Make sure you have support for all abdominal exercises you do – meaning a sheet wrapped around your abdomen or you can just grab the edges of the rectus abdominis and make sure they stay together with the exercises.
If the muscles are not coming together in 6-8 weeks, I would visit a women’s health physical therapist. Scar tissue is laid down anytime a surgeon cuts into the body, and especially with abdominal surgery, the scar tissue may be preventing the muscles from coming together in the front. The fiber orientation of scar tissue is disorganized and laid down in a random manner, meaning it can attach to anything around it – skin, muscle, bone, organs, etc. This can result in adhesions that inhibit normal gliding of the surrounding organs and normal contraction of abdominal/pelvic/hip musculature. Without manual intervention to break up the scar tissue, it may be difficult for the muscles to return to a better resting position.
Get help now from a pelvic floor therapist
Question:
I had a cesarean section and am having difficulty engaging my abdominal muscles. I think I also may have a diastasis in my lower abdominals. Does having a cesarean section affect which exercises I should be doing and my recovery rate? Thank you so much!
– E.K., CA
Answer:
I am so glad you asked this question as there is a huge population of women who have had cesarean sections. Scar tissue is also an issue with this population and can restrict the abdominal muscles from gliding normally. The abdominal muscles and fascia are sewn back together following the operation and it takes 6-8 weeks for the muscles to heal – meaning you should not begin an abdominal exercise program for 6-8 weeks (you must receive clearance from your Obstetrician first). Scar tissue will be laid down along the entire depth of the incision line and will decreased tissue glide unless the issue is addressed. This may prolong or prevent correct muscle activation and can therefore affect proper closing of the diastasis recti. The exercises for women with cesarean sections are the same, but if you notice that your muscles are not coming back to midline within 6-8 weeks following the start of the exercises, then you may want to consider seeing a women’s health physical therapist.
Question :
I had twins 6 months ago and am still struggling with looking pregnant. I have a moderate separation above, at and below my belly button. I have being doing exercises for diastasis recti for a month now and I think my muscles are slowly coming back together. Should I be wearing an abdominal binder to help with the process? Also – I think my TA, the muscle on the inside of my hip bone, is starting to hurt from working it so hard. Is that normal? Thanks for your help!
– R.M., NY
Answer :
For a moderate to significant separation (> 6 cm separation at rest), an abdominal binder can definitely be useful. The binder helps with preventing further separation of the abdominal muscles during functional activities, such as lifting your child and pushing a stroller, by providing external passive splinting of the muscles. You should wear the binder during the day when you are doing physical activities and only if you are also doing abdominal exercises without the binder. If you rely on the binder, the muscles will become weak and your separation will not come back together. While wearing the binder, you don’t have to actively hold in your abdominals. The splint should bring the two ends of the muscles together so that when you need to engage your abdominals (lifting, pushing) they are in a good, safe position. The muscle just inside your hip bones are either your obliques or Transverses Abdominis – neither should be getting sore with the exercises. Make sure you are not constant holding in your abdominals throughout the day with the binder and that you are only lightly contracting the TA with the exercises (your buttocks and superficial abdominals should not be contracting).
Question :
What does “women’s health physical therapy†mean and how does it differ from regular physical therapy? If I have issues surrounding my pregnancy, can’t I just go into any physical therapy clinic?
– C.W., FL
Answer:
Great question! To be honest, “women’s health†is an outdated term since many of these clinics also treat men and children. The term is now shifting to “pelvic floor physical therapist.†I specifically used the term women’s health because many general orthopedic PT clinics that don’t treat pelvic floor issues do treat pre- and post-partum women. If you are interested in physical therapy services, be sure to call the clinic and ask if there is anyone there who specializes in pre- or post-partum care.
I specifically work as a pelvic floor physical therapist treating varying orthopedic conditions, women’s health issues and bowel, bladder and sexual dysfunction in men and women. Typical diagnoses that I treat are painful sex, painful urination, urinary frequency, urinary urgency, urinary incontinence, interstitial cystitis, endometriosis, pre/post-partum, rectal pain, constipation, fecal incontinence, lower back/coccyx/pelvic/sacral pain and any post-op abdominal, back, hip, pelvic or bowel/bladder/vaginal surgery. Pelvic floor refers to the group of muscles that sling from your pubic bone in the front to your coccyx bone in the back. Since three different systems (Bowel, Bladder & Sexual) go through these muscles any pelvic mal-alignment, weakness, tightness or dysfunction in coordination can disturb any or all three systems. If you remember back to the analogy of the core as a closed canister, any dysfunction in these muscles can affect breathing, abdominal organ function, trunk stability and in turn the extremities that rely on the trunk for stability.
Again, if you continue to have any questions or concerns, please email me at [email protected] or visit our clinic website to schedule an appointment: https://beyondbasicsphysicaltherapy.com