Joint Hypermobility and Hypermobility Spectrum Disorders (HSD)

What is Joint Hypermobility?
Joint hypermobility means your joints move farther than what is typical. Some people feel flexible without any discomfort, while others experience pain, stiffness, or a sense that their joints feel loose or unstable. Joint hypermobility can exist on its own or as part of a wider pattern of symptoms seen in Hypermobility Spectrum Disorders.
- Joints that move past a normal range
- A feeling of looseness or slipping in the joints
- Muscle or joint pain during or after activity
- Muscle or joint stiffness due to overcompensation
- Frequent strains or sprains
- Fatigue, especially after tasks that require stability
- Clumsiness or poor balance
- Digestive or pelvic floor concerns related to connective tissue laxity


What are Hypermobility Spectrum Disorders?
Hypermobility Spectrum Disorders are connective tissue conditions that involve joint hypermobility along with a range of symptoms that affect daily life. Even though the name might sound mild, HSD can cause significant discomfort, frustration, and functional challenges.
HSD sits within a group of conditions related to joint hypermobility, but without a clear genetic pattern. People with HSD often feel unheard or confused by their symptoms, especially when medical tests come back normal.
Get help with pelvic floor physical therapist for HSD and joint hypermobility.
Symptoms of HSD
The symptoms of HSD can include:
- Joint hypermobility
- Muscle and joint pain
- Fatigue
- Gastrointestinal issues
- Pelvic floor dysfunction
- Joint instability or frequent sprains
- Autonomic symptoms like dizziness or fast heart rate when standing
- Anxiety, which can be worsened by the unpredictability of symptoms

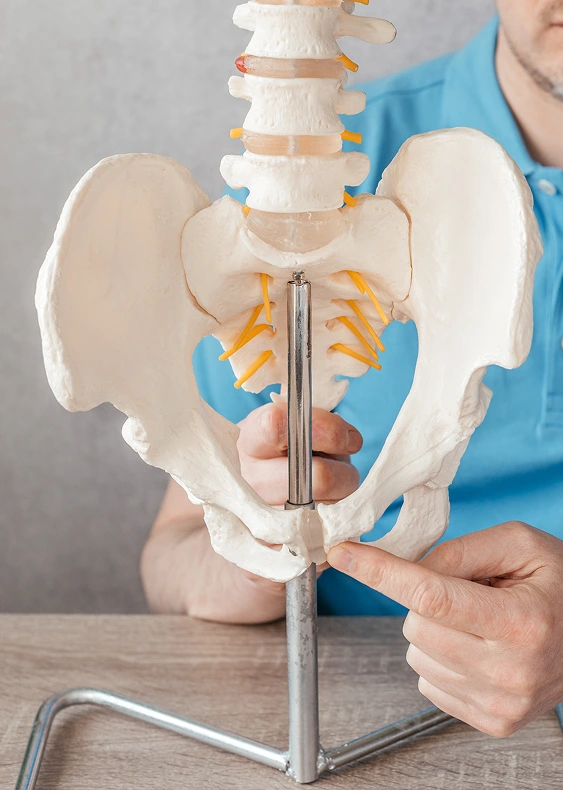
How HSD, Joint Hypermobility, and Pelvic Floor Dysfunction Are Connected
Pelvic floor dysfunction often appears in people with HSD or joint hypermobility, yet many do not receive a clear explanation at first. They move from provider to provider without answers, even though their symptoms often relate to how their connective tissue behaves.
The pelvic floor muscles and connective tissue support the bladder, bowel, and reproductive organs. When that tissue lacks stability, as it often does with HSD or joint hypermobility, the pelvic floor works harder to create support. This extra effort can lead to tension, weakness, poor coordination, and pain.
You might notice:
- Pelvic organ prolapse
- Incontinence or sudden urgency to urinate
- Constipation or discomfort with bowel movements
- Pain during sex or pelvic exams
- A feeling of abdominal pressure or bloating
- Lower back, hip, or tailbone pain
Many people with HSD or joint hypermobility also experience conditions like Irritable Bowel Syndrome (IBS), Mast Cell Activation Syndrome (MCAS), or Postural Orthostatic Tachycardia Syndrome (POTS). These conditions can influence how the pelvic floor reacts by affecting the nervous system, digestion, and overall tissue comfort.
Pelvic floor physical therapy helps calm the nervous system, improve coordination, and support steadier movement patterns. It focuses on understanding how your body responds, how it compensates, and what helps you feel more supported day to day.
How is HSD and Joint Hypermobility Diagnosed?
Providers diagnose HSD and joint hypermobility through a clinical evaluation that looks at your medical history, your physical symptoms, and joint mobility. There is no single test that confirms HSD or joint hypermobility, so clinicians use structured criteria that assess how far your joints move, how your symptoms show up in daily life, and whether other conditions could explain what you are feeling. When your joints move beyond a typical range and you experience related symptoms without meeting criteria for another connective tissue condition, a provider often diagnoses HSD.

Treatment for HSD and Hypermobility
Your first visit focuses on listening. Your therapist will ask about your symptoms, history, goals, and how pain affects your daily life. Nothing is rushed.
Your therapist might assess posture, breathing, hip mobility, and pelvic muscle function. A physical exam may be included if appropriate, always guided by your consent. You can pause or decline any part of the session. You will leave with simple tools and exercises designed to help your body begin relaxing and retraining between visits.
Pelvic Floor Physical Therapy
We assess how your pelvic floor muscles are functioning and work to improve coordination, reduce tension, and address issues like prolapse, urgency, or pain with sex.
Stability and Strength Training
Myofascial and Trigger Point Release
Pain Management
Client Testimonials
Get help now from a pelvic floor therapist for HSD and joint hypermobility.
Beyond Basics: We Can Help
Since 2003, Beyond Basics has been a place of hope and healing for our patients. We believe skilled and compassionate healing can restore your body’s harmony and balance. Founder, Amy Stein, and co-founder, Corey Hazama are renowned experts and leaders in pelvic floor PT.
The skilled physical therapists at Beyond Basics receive extensive training to qualify them to be the world’s leaders in pelvic floor rehabilitation. All of our therapists have been carefully selected to work at Beyond Basics because they possess the right expertise, kindness, and empathy to allow them to excel at our practice. Our therapists have completed hundreds of additional hours outside of their doctorates both internally and externally through institutes such as Herman and Wallace and the American Physical Therapy Association, to help hone their practice and provide exceptional treatment efficiently and compassionately. In addition to being the world’s first and foremost experts in pelvic floor dysfunction, our individual therapists have cultivated additional skills unique to their own personal interests. Read more about each one of our therapists here.


